Preparing for the worst: Valley Medical Center staff preps for possibility of Ebola
Published 12:39 pm Friday, October 24, 2014
Valley Medical Center is screening all patients for potential Ebola exposure coming to its clinics, the emergency room or hospital as it responds to the outbreak of the deadly disease in West Africa.
It’s unlikely that anyone in South King County will become infected, but hospital officials and the rest of the medical establishment in King County are preparing to respond to one case or many.
“We all just have to be vigilant,” said Dr. Kathryn D. Beattie, Valley Medical’s chief medical officer.
Part of Valley’s response is educational and a chance to remind everyone that their well-being is in their hands.
“The two most important things that they can do to promote their own well-being would be to wash their hands and get their flu shots,” said Beattie, pointing out there’s a “much higher likelihood” of getting seriously ill from the flu than contracting Ebola.
 Ebola is only transferred through contact with bodily fluids, including from a sneeze, and not casually, such as when sitting with someone on a plane or in a movie theater, Beattie said.
Ebola is only transferred through contact with bodily fluids, including from a sneeze, and not casually, such as when sitting with someone on a plane or in a movie theater, Beattie said.
The vigilance extends from training and drilling hospital staff on the proper way to put on and take off protective equipment when determining whether a patient has Ebola – or any infectious disease – to asking patients about their travels at registration.
Patients are asked whether they’ve traveled outside the country in the last 21 days – the incubation period for Ebola – and whether they’ve been in the West African countries of Guinea, Liberia and Sierra Leone, the hardest hit by the disease.
The questions are asked when making an appointment or a person registers in person at a Valley Medical facility.
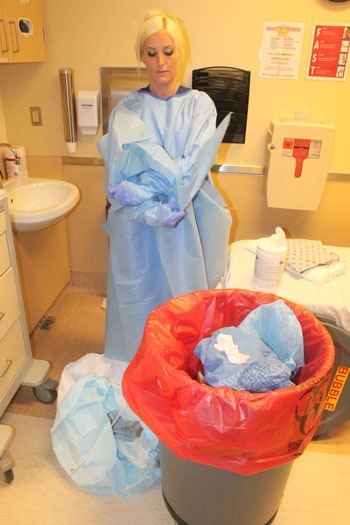
If the answers are yes, the patient is given a mask and placed in a sparsely appointed isolation room, where hospital staff, dressed in four layers of Personal Protective Equipment, ask more questions about symptoms and travel and examine the patient to determine whether the patient is at risk.
Public Health – Seattle and King County is involved in this in-depth screening, which follows the protocols of the national Centers for Disease Control.
The protocol was followed late last week when a patient arrived at Valley’s emergency room. He was asked whether he had traveled to Africa in the last 21 days. He answered yes and also responded yes when asked whether he had these symptoms – nausea, vomiting and diarrhea.
In asking more questions the staff determined he had traveled to Ethiopia, not one of the affected African countries. Registration personnel had not specifically asked whether he had traveled to West Africa. The patient likely had a bad cold.
But the experience helped hospital personnel refine their procedures and tested how well the isolation room worked, according to Theresa Braungardt, Valley’s chief nursing officer, who responded to the incident.
“It kind of became a drill,” she said.
A suspected case of Ebola is confirmed through a blood test before a patient is placed in one of two isolation rooms in the actual hospital. Harborview Medical Center, which like Valley is also part of UW Medicine, has two isolation rooms.
This week, all staff members in Valley’s Emergency Department received training in the use of the protective gear. Staff at Valley’s primary care clinics have been trained as well; the clinics received standardized kits with the equipment and have designated their own isolation rooms.
Hospitals across the country learned from the fate of two nurses who contracted Ebola at the Dallas hospital where Thomas Eric Duncan, the nation’s first confirmed Ebola case, was treated and then died Oct. 8. The nurses are recovering, but health professionals learned the gear didn’t protect their neck and facial areas.
Valley’s protective equipment includes a plastic capper with a shroud that covers a staffer’s neck and face. CDC’s protocols continue to evolve, too. Earlier this week, the CDC recommended that hospital personnel not wear goggles because of the potential to contaminate themselves when they wipe off the steam.
 Roz Currie Parsons, staff nurse in the emergency room, this week demonstrated how to put on and take off the protective gear. She was observed and when necessary assisted by Celeste Etherington, clinical nurse specialist. In a real-life situation, Etherington would wear the protective gear, too; they would dress in a room next to the isolation room.
Roz Currie Parsons, staff nurse in the emergency room, this week demonstrated how to put on and take off the protective gear. She was observed and when necessary assisted by Celeste Etherington, clinical nurse specialist. In a real-life situation, Etherington would wear the protective gear, too; they would dress in a room next to the isolation room.
“We take the protection of our staff very, very seriously,” said Kayett Asuquo, the director of Valley’s Emergency Department.
Parsons has talked with her family about the potential she might treat a patient with Ebola.
“I have communicated it to my family that if there was a case, then I would be isolating myself,” said Parsons, who has helped teach the safety classes.
Taking off the impermeable gear is a critical part of the process, because this is when contamination could occur. Bleach is used to clean gloves and hands are frequently washed; the gowns are double-bagged before disposal, which in real life is done by a specialized contractor.
Even if there isn’t a case of Ebola again in the United States, the protocols developed and refined to respond to the disease will better prepare the nation’s medical community to respond to a similar outbreak of an infectious disease, such as the flu, say Beattie and Braungardt.
“I would say that across the board what we are seeing is that overall for our staff and for their community there is a heightened awareness of infection prevention techniques and how important it is to follow them to the T,” said Beattie. That means washing hands and getting a flu shot.